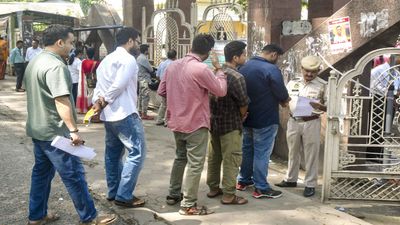The recent surge in H5N1, commonly known as bird flu, infections in both wild and domestic birds, alongside cases appearing in dairy cattle across several U.S. states and horses in Mongolia, has raised alarms. This flu variant, already linked to 61 human cases in the U.S. this year—mostly among farm workers exposed to infected cattle and individuals consuming raw milk—marks a significant uptick from only two reported cases in the Americas over the past two years. Given its 30% mortality rate among humans, health officials are increasingly prioritizing H5N1's containment. Despite its current inability to transmit from person to person, limiting its pandemic potential, the situation underscores the constant vigilance required to monitor and manage infectious diseases.
In the face of COVID-19's devastating impact, the world remains on high alert for the next major infectious threat. Diseases such as malaria, HIV, and tuberculosis, which collectively claim around 2 million lives annually, continue to pose significant challenges. Moreover, the rise of pathogens resistant to conventional treatments, like antibiotics and antivirals, adds another layer of complexity to public health efforts. Among the various pathogens under scrutiny, influenza viruses, particularly the A subtype H5N1 or bird flu, stand out due to their potential for rapid spread and mutation.
One of the most concerning aspects of H5N1 is its capacity to infect humans, as evidenced by the recent spike in cases in the U.S. Historically, bird flu has not been able to spread easily between humans due to its preference for avian sialic receptors over human ones. However, research suggests that a single genetic mutation could enable H5N1 to overcome this barrier, potentially triggering a human pandemic. In response, countries have prepared by developing pandemic plans and stockpiling vaccines; the UK, for instance, has acquired 5 million doses of an H5 vaccine in anticipation of future outbreaks.
Despite these efforts, the broader implications of bird flu, particularly on animal health and welfare, cannot be overlooked. The expected increase in H5N1 cases among animals by 2025 poses significant risks to food security and economic stability, highlighting the interconnectedness of human, animal, and environmental health. This concept, known as "one health," emphasizes the importance of a holistic approach to disease prevention and management.
The battle against infectious diseases is far from over, with ongoing threats like malaria, HIV, and tuberculosis demanding continuous attention. As the world navigates the aftermath of COVID-19 and braces for future challenges, the importance of integrated health strategies becomes ever more apparent. By prioritizing the health of our environment and animal populations, we can better safeguard against the emergence of new diseases and mitigate the impact of existing ones. However, the potential for an H5N1 pandemic, driven by a mere genetic shift, serves as a stark reminder of the need for readiness and resilience in the face of infectious disease threats.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications