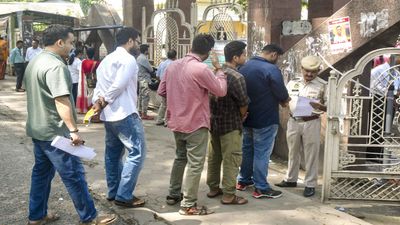A blood test could predict if a person infected with the SARS-CoV-2 virus will develop long COVID, a study published in the Lancet eBioMedicine journal suggests. Some people who have been infected with COVID-19 experience long-term effects from their infection, known as long COVID.
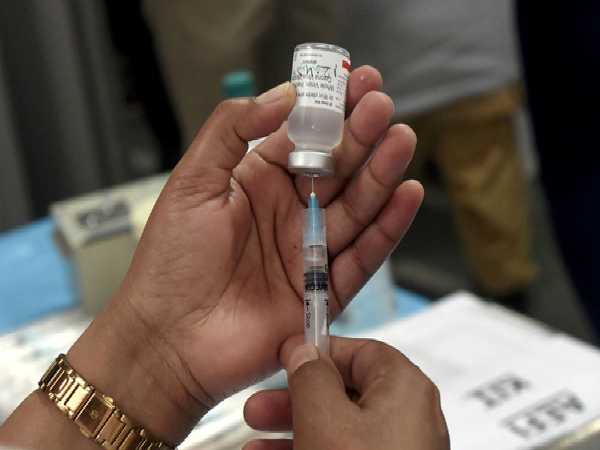
The researchers at University College London (UCL) in the UK analysed proteins in the blood of health care workers infected with SARS-CoV-2, comparing them to samples from those who had not been infected. They found a dramatic difference in levels of some of the proteins up to six weeks following infection, suggesting disruption to a number of important biological processes. Using an artificial intelligence (AI) algorithm, the team identified a "signature" in the abundance of different proteins that successfully predicted whether or not the person would go on to report persistent symptoms a year after infection. The researchers said that, if these findings are repeated in a larger, independent group of patients, a test could potentially be offered alongside a polymerase chain reaction (PCR) test that could predict people's likelihood of developing long COVID.
"Our study shows that even mild or asymptomatic COVID-19 disrupts the profile of proteins in our blood plasma," said study lead author Gaby Captur from UCL. "This means that even mild COVID-19 affects normal biological processes in a dramatic way, up to at least six weeks after infection," Captur said. The method of analysis used in the study is readily available in hospitals and is high-throughput, meaning it can analyse thousands of samples in a short time. "If we can identify people who are likely to develop long COVID, this opens the door to trialling treatments such as antivirals at this earlier, initial infection stage, to see if it can reduce the risk of later long COVID," said study senior author Wendy Heywood from UCL.
The researchers analysed blood plasma samples from 54 health care workers who had PCR- or antibody-confirmed infection, taken every week for six weeks in spring 2020. They compared the samples with those taken over the same period from 102 health care workers who were not infected. The researchers used targeted mass spectrometry, a form of analysis that is extremely sensitive to tiny changes in the amount of proteins in blood plasma, to look at how COVID-19 affected these proteins over the course of six weeks. They found abnormally high levels of 12 proteins out of the 91 studied among those infected by SARS-CoV-2.
The team found that at the time of first infection, abnormal levels of 20 proteins studied were predictive of persistent symptoms after one year. Most of these proteins were linked to anti-clotting and anti-inflammatory processes.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications